Introduction
Blood banks are vital pillars of modern healthcare, providing safe blood and its components for patients in need. Ensuring the quality, safety, and functionality of blood products requires the use of specialized equipment and strict adherence to global standards. This comprehensive article highlights the essential types of blood bank equipment, optimal storage conditions, processing procedures, and key best practices for maintaining the safety of blood.

Understanding Blood Components and the Importance of Proper Storage
Whole blood consists of four primary components, each with a distinct function:
Plasma: Transports nutrients, hormones, proteins, and waste products.
Red Blood Cells (RBCs): Carry oxygen to tissues and remove carbon dioxide.
White Blood Cells (WBCs): Defend the body against infections.
Platelets: Aid in clotting and tissue repair.
After donation, blood is separated into its components using centrifugation. Each component must be stored under specific conditions to preserve its viability and effectiveness.
Blood Component Storage Temperatures and Shelf Life
| Blood Product | Storage Temperature | Shelf Life |
|---|---|---|
| Whole Blood & RBCs | +2°C to +6°C | 35–42 days (depending on additives) |
| Platelets | +20°C to +24°C with agitation | 5–7 days |
| Frozen Plasma | ≤ -30°C | Up to 12 months |
| Frozen RBCs | -65°C or colder | Up to 10 years |
| Granulocytes (a type of WBC) | Room temperature | Usable within 24 hours |
Any deviation from these temperature ranges can cause contamination, degradation, or loss of therapeutic function

Essential Blood Bank Equipment and Their Functions
1. Blood Collection Devices
Collection Monitors: Ensure steady blood flow and mixing to prevent clotting.
Apheresis Machines: Extract specific blood components (e.g., plasma, platelets) directly from the donor.
2. Blood Processing Equipment
Centrifuges: Separate blood components by density.
Automated Processing Systems: Improve efficiency and reduce human error.
Plasma Thawers: Safely thaw frozen plasma while maintaining sterility.
3. Storage Equipment
Blood Bank Refrigerators: Maintain +2°C to +6°C for RBCs and whole blood with precise temperature control, alarms, and data logging.
Plasma Freezers & ULT Freezers: Store plasma and cryopreserved cells at -30°C to -86°C.
Platelet Agitators & Incubators: Preserve platelet viability with consistent motion at room temperature.
4. Testing and Quality Control
Automated Analyzers & Microplate Readers: Screen for infectious diseases and ensure product quality.
Hemovigilance Systems: Monitor adverse events and improve transfusion safety protocols.
5. Transportation Systems
Insulated Boxes & Refrigerated Vehicles: Maintain cold chain integrity during distribution.
Tracking-Enabled Transport Containers: Provide real-time monitoring and compliance with international regulations.
6. Temperature Monitoring Tools
Wireless Monitoring Systems: Offer 24/7 real-time tracking with alerts for any temperature deviations.
The Blood Cold Chain: A Lifesaving Continuum
The blood cold chain is the uninterrupted maintenance of appropriate temperatures for blood from donation to transfusion. Any break in this chain renders the blood unsafe and unusable. Modern equipment ensures this continuum is preserved and reliable.
Best Practices for Safe Blood Handling
Continuous temperature monitoring with alert systems
Regular equipment calibration and servicing
Comprehensive staff training
Backup power systems
Sterile equipment cleaning routines
FIFO inventory management
Barcode labeling and digital record-keeping
Use of standardized handling protocols
Adherence to national and international standards
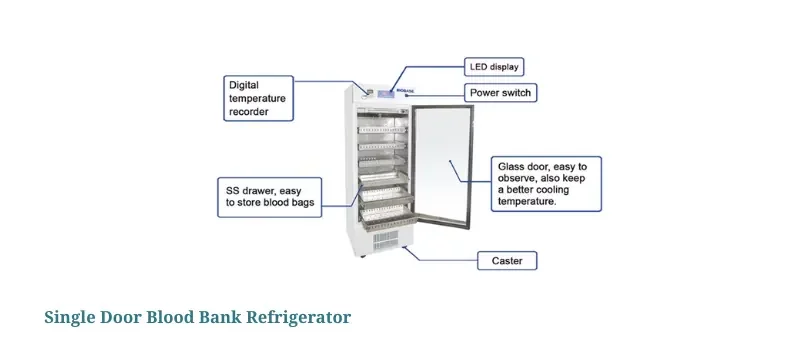
Selecting the Right Equipment for Your Facility
Choosing the proper equipment depends on:
Volume of donations
Storage needs
Types of blood components processed
Space and budget constraints
Local regulatory requirements
AELAB provides customizable equipment ranging from compact refrigerators to advanced freezing systems, tailored for hospitals, blood centers, and mobile units.
Conclusion
Blood bank equipment is more than just technology—it’s a cornerstone of patient safety. With advanced systems for collection, processing, storage, and transportation, and by complying with rigorous standards, blood banks can ensure high-quality transfusion services. Investing in certified, reliable equipment is not only a legal obligation but a moral imperative to save lives and support public health.





















