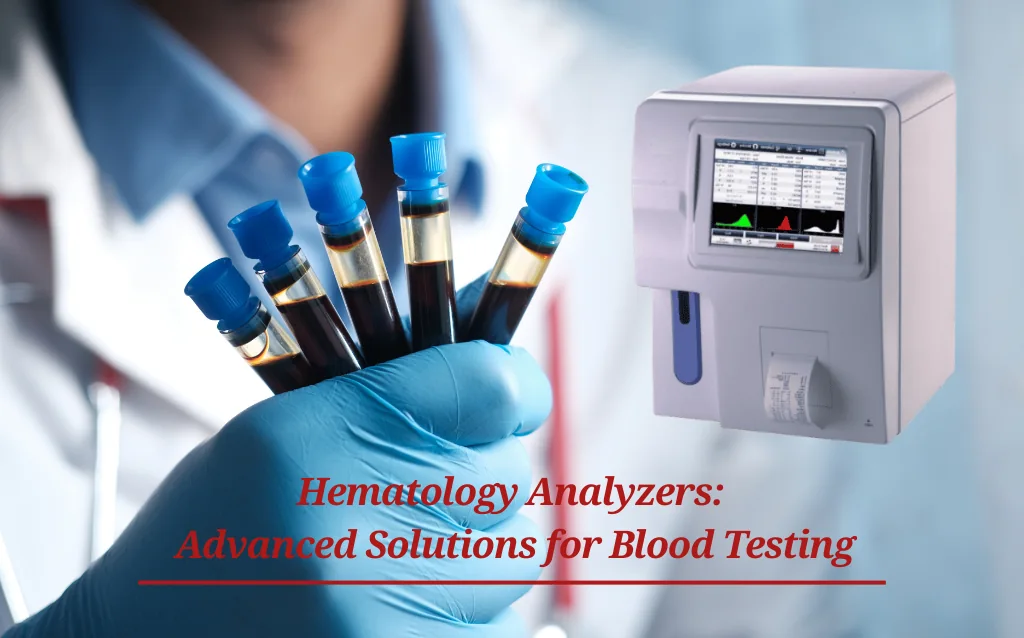
Introduction: Blood as the Key to Precision Medicine
In today’s rapidly advancing medical landscape, blood is more than just a vital fluid—it’s a data-rich substance that offers critical insights into a patient’s health. Hematology analyzers have become indispensable in this process, helping clinicians diagnose anemia, infections, cancers, and chronic diseases with precision and speed. Blood analysis now plays a pivotal role in clinical decision-making.
To meet the growing demand for fast, reliable, and accurate diagnostics, automated hematology analyzers have revolutionized the way laboratories process blood samples. These advanced devices empower healthcare professionals with high-throughput, high-precision testing that forms the backbone of modern diagnostics.

What Is a Hematology Analyzer?
A hematology analyzer is a laboratory instrument designed to perform Complete Blood Count (CBC) tests and other blood analyses by counting, classifying, and measuring various blood cell components.
Core Parameters Measured:
Red Blood Cells (RBCs): Count, Hemoglobin (Hb), Hematocrit (HCT), MCV, MCH, RDW
White Blood Cells (WBCs): Total count, 3-part or 5-part differential, abnormal flags
Platelets (PLTs): Count, MPV, PDW
Additional Metrics: Reticulocytes, NRBCs, and cell morphology in advanced models
How Do Hematology Analyzers Work?
Hematology analyzers rely on automated technologies to analyze blood samples efficiently and accurately. The three primary methods used are:
1. Electrical Impedance (Coulter Principle)
Measures electrical resistance as cells pass through a narrow aperture, determining cell size and count.
2. Flow Cytometry
Uses laser beams and fluorescent markers to analyze multiple parameters such as cell type, granularity, and surface markers in real time.
3. Optical or Spectrophotometric Methods
Measures light absorption or scattering to assess cell properties like shape, internal complexity, and hemoglobin concentration.
Types of Hematology Analyzers
By WBC Differentiation:
3-Part Differential: Distinguishes lymphocytes, monocytes, granulocytes—suitable for routine tests.
5-Part Differential: Offers full classification into neutrophils, lymphocytes, monocytes, eosinophils, and basophils.
Advanced Analyzers: Include reticulocyte count, NRBCs, and integration with Laboratory Information Systems (LIS).
By Format and Capacity:
Fully Automated Analyzers: High-throughput systems for busy hospital labs.
Semi-Automated Analyzers: Require manual sample loading; ideal for medium-volume labs.
Point-of-Care (POC) Devices: Portable, user-friendly units for clinics and remote locations.
Integrated Systems: Combine hematology with clinical chemistry or immunoassay modules.
Key Advantages of Automated Hematology Analyzers
| Feature | Manual Analysis | Automated Analyzer |
|---|---|---|
| Speed | Low | High throughput |
| Accuracy | Operator-dependent | Standardized & algorithm-based |
| Parameter Range | Limited | Comprehensive |
| Operator Skill Needed | High | Low to moderate |
| Consistency | Variable | Highly reproducible |
Benefits at a Glance:
Speed & Efficiency: Capable of processing hundreds of samples per hour.
Accuracy & Objectivity: Reduces human error and inter-operator variability.
Comprehensive Data: Delivers a broad panel of hematological metrics.
Minimal Intervention: Automates everything from sampling to result reporting.
Clinical & Research Applications
Hematology analyzers are indispensable across a variety of healthcare and research environments:
Clinical Diagnostics: Identifying anemia, leukemia, thalassemia, infections, and clotting disorders.
Treatment Monitoring: Assessing chemotherapy effectiveness and bone marrow recovery.
Blood Banking: Screening donors for safe transfusions.
Scientific Research: Supporting studies in immunology, hematology, and public health.
How to Choose the Best Hematology Analyzers
Choosing the right hematology analyzer depends on specific clinical and operational requirements. Consider the following factors:
Lab Size & Sample Volume
Small labs: Compact 3-part analyzers
Mid-to-large labs: 5-part or fully automated systems
Test Requirements
Routine CBC: Basic model
Specialized testing: Advanced units with reticulocyte/NRBC analysis
Automation & Integration
LIS compatibility, autoloaders, cloud connectivity
Ease of Use
Touchscreen interface
Minimal training and maintenance
Regulatory Compliance
Look for CE, FDA 510(k), ISO, CLIA certifications
Cost Efficiency
Total cost of ownership (TCO) including reagents and service contracts
Consider open reagent systems
Space & Infrastructure
Match analyzer size with available lab space
Check power, ventilation, and environmental needs

Pro Tips for Optimal Performance
Use certified, high-quality reagents
Schedule regular maintenance and calibration
Train staff to recognize system flags
Document quality control procedures
Utilize vendor support for software and technical updates
Emerging Trends & Future Outlook
The field of hematology analysis is evolving with the integration of cutting-edge technologies:
Future Directions:
AI-Powered Diagnostics: Improved pattern recognition and predictive capabilities
Remote Monitoring: Real-time performance insights via cloud platforms
Decentralized Testing: Portable, benchtop analyzers for remote and low-resource areas
Sustainable Design: Energy-efficient and environmentally friendly systems
Personalized Medicine Integration: Tailored diagnostics aligned with patient-specific treatment
Conclusion: Investing in Precision and Efficiency
Hematology analyzers are foundational to accurate blood diagnostics in modern healthcare. By understanding their features, technologies, and benefits, laboratories can make informed decisions that enhance both clinical outcomes and operational productivity.
Whether you’re equipping a small clinic or a high-volume hospital lab, choosing the right hematology analyzer is a strategic move toward faster, smarter, and more reliable diagnostics.